Password Reset
Forgot your password? Enter the email address you used to create your account to initiate a password reset.
Forgot your password? Enter the email address you used to create your account to initiate a password reset.
4 Minutes
Michael R. Czachowski, MBA, CNMT, NCT, PET, ASCP(N), R.T.(N)(BD) (ARRT), is the supervisor of the Nuclear Medicine and Molecular Imaging Departments. He explains that UPMC Children’s Hospital of Pittsburgh was the first facility in the United States to perform portable Xenon-133 lung ventilation exams on patients in the pediatric cardiac intensive care unit (CICU). “This is an extremely innovative process that was devised to allow us to perform the ventilation lung exams using the Digirad Ergo™ portable nuclear camera on the most medically fragile patients without having to move them to the nuclear medicine department,” says Mr. Czachowski.
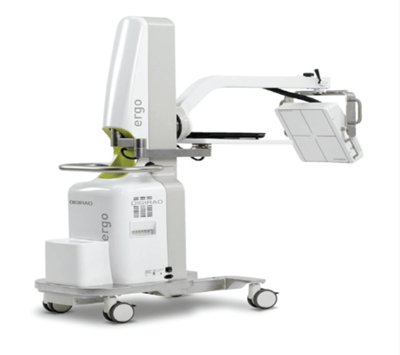
The journey for developing this process beganin the CICU while performing a portable perfusion lung exam on a patient. A CICU physician asked Mr. Czachowski and his team if there was a possibility of also performing a portable ventilation lung exam on patients in the intensive care units. The current standard of practice in performing ventilation lung scans in nuclear medicine is through the use of Tc-99m DTPA (diethylenetriamine pentaacetic acid) aerosol. However, as Mr. Czachowski points out, “using an aerosol for these critically ill patients in the CICU is not an option due to the inability to deliver the aerosol and the possibility of radiation contamination.”
“The first option that came to mind was to perform the portable ventilation lung exams using a Krypton-81m gas generator. After some research, it was determined that the generators were no longer available in the United States. Because of this, we had to explore other options. This eventually led to the idea of using Xenon-133 gas in conjunction with the patient’s ventilator and our Pulmonex system,” says Mr. Czachowski. The Pulmonex system is used in the nuclear medicine department to perform Xenon-133 lung ventilations exams. The system is designed to safely capture the exhaled Xenon-133 into a lead-lined trap.
“The challenge was to find a way to perform the exam on patients in the CICU who are ventilator-dependent without removing them from the device or transporting them to the nuclear medicine department. Because Xenon-133 is a radioactive gas that would be exhaled by the patient during the exam, we had to think of how to capture the gas from the patient into the Pulmonex system, while ensuring a safe environment for the patient, family, and staff,” says Mr. Czachowski.
Mr. Czachowski collaborated closely with Alvin Saville, RRT, who is the respiratory education coordinator at UPMC Children’s. They developed a way to keep the patient on the ventilator and administer the Xenon-133 gas through a tubing adaption placed between the patient’s endotracheal tube and the ventilator circuit. The exhaled radioactive Xenon-133 gas is then safely trapped in the Pulmonex system upon exhalation.
The system was used for the first time on a patient in April 2018 after months of development and testing in the Nuclear Medicine Department by Mr. Czachowski and his collaborators. They continue to refine the protocol and look for new ways to use the technology to expand the ability to help clinicians and patients across the hospital.
“You have to remember these are critically ill patients. To do the lung ventilation exam with no interruption of the patient’s physiological and physical environment in the CICU or elsewhere is quite an accomplishment. We have developed a seamless process that is safe and efficient,” says Mr. Czachowski.
“We could always perform perfusion lung exams portably in the intensive care units with our Digirad Ergo, but now with this new approach, we can add the ventilation lung exam with no disruption in the environment of the patient. This additional piece of information provided by the ventilation exam can be critical in the clinical decisions made for the patient. The importance of such collaboration and innovation can lead to better patient outcomes,” says Mr. Czachowski.
There are certain conditions where a perfusion exam may be normal but an accompanying ventilation exam may show abnormalities. The lung ventilation exams can help determine whether the patient needs an additional procedure and, if so, what procedure. Some procedural examples are cardiac catheterization or a bronchoscopy. The additional information provided by the lung ventilation exam can help to narrow down and guide the best course of treatment. “This is where the importance of such an innovative way of doing these tests really shows up. The right treatment for the right patient at the right time.”