Password Reset
Forgot your password? Enter the email address you used to create your account to initiate a password reset.
Forgot your password? Enter the email address you used to create your account to initiate a password reset.
4 Minutes
Older people who report greater levels of social engagement have more robust gray matter in regions of the brain relevant in dementia, according to new research led by scientists at the University of Pittsburgh Graduate School of Public Health. It is the first to use a particularly sensitive type of brain imaging to conduct such an evaluation.
The findings, reported today in the Journal of Gerontology: Psychological Sciences, suggest that “prescribing” socialization could benefit older adults in warding off dementia, much the way prescribing physical activity can help to prevent diabetes or heart disease.
 “Our data were collected before the COVID-19 pandemic, but I believe our findings are particularly important right now, since a one-size-fits-all social isolation of all older adults may place them at risk for conditions such as dementia,” said lead author Cynthia Felix, MD, MPH, a geriatrician and a post-doctoral associate in Pitt Public Health’s Department of Epidemiology. “Older adults should know it is important for their brain health that they still seek out social engagement in safe and balanced ways during the pandemic.”
“Our data were collected before the COVID-19 pandemic, but I believe our findings are particularly important right now, since a one-size-fits-all social isolation of all older adults may place them at risk for conditions such as dementia,” said lead author Cynthia Felix, MD, MPH, a geriatrician and a post-doctoral associate in Pitt Public Health’s Department of Epidemiology. “Older adults should know it is important for their brain health that they still seek out social engagement in safe and balanced ways during the pandemic.”
Felix and her colleagues used information about social engagement from 293 community-dwelling participants from the Health, Aging and Body Composition (Health ABC) study. These participants, who averaged 83 years old, also received a sensitive brain scan called Diffusion Tensor Imaging MRI that measured the cellular integrity of brain cells used for social engagement.
These participants provided detailed information about their social engagement and were scored using a tool Felix developed. High scores were awarded to people who did things like play board games; go to movies; travel long distance; attend classes, lectures or adult education events; participate in church or other community activities; get together with children, friends, relatives or neighbors at least once a week; volunteer or work; be married and live with others.
Felix and colleagues found that greater social engagement is related to better microstructural integrity of brain gray matter in these older adults. Maintaining brain health is of critical importance. Once brain cells die, dementia typically follows.
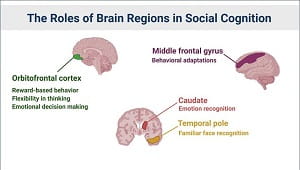 Social engagement with at least one other relative or friend activates specific brain regions needed to recognize familiar faces and emotions, make decisions and feel rewarded. The good news is that even moderate “doses” seem to be beneficial.
Social engagement with at least one other relative or friend activates specific brain regions needed to recognize familiar faces and emotions, make decisions and feel rewarded. The good news is that even moderate “doses” seem to be beneficial.
“We need to do more research on the details, but that’s the beauty of this—social engagement costs hardly anything, and we do not have to worry about side-effects,” Felix said. “There is no cure for dementia, which has tremendous costs in terms of treatment and caregiving. Preventing dementia, therefore, has to be the focus. It’s the ‘use it or lose it’ philosophy when it comes to the brain.”
Felix notes that cause-and-effect still need to be disentangled: Does greater social engagement keep these brain regions healthy? Or is it that having a healthy brain results in better social engagement?
Similar to how large public health studies assess the best programs to encourage physical activity to prevent chronic disease in older people, Felix believes her team’s findings, coupled with previous research, provides justification for randomized control trials to assess the impact of specific types and amounts of social activities on brain health.
Enriched by her prior public health training at Johns Hopkins University, Felix recognizes the critical role of public health in applying this finding on a large scale.
“It would be good if we develop programs across the U.S. through which structured social activities can be prescribed for community-dwelling older adults, aimed at reducing rates of dementia and the resulting health care costs,” Felix said. “Existing platforms providing group physical activities can be a good starting point.”
Additional authors on this research are Caterina Rosano, MD, MPH, Xiaonan Zhu, PhD, and Andrea L. Rosso, PhD, MPH, all of Pitt; and Jason D. Flatt, PhD, MPH, of the University of Nevada, Las Vegas.
This research was supported by National Institutes of Health (NIH) contracts N01-AG-6-2101, N01-AG-6-2103 and N01-AG-6-2106, NIH grants R01-AG-028050, R01-NR-012459, K23-AG-028966 and R01-AG-029232, and University of Pittsburgh Claude D. Pepper Older Americans Independence Center grant P30-AG-024827-07.